
What is Tinea Capitis? How to manage it? What are the precautions to be taken? What are the signs and symptoms? What is the cause of this disease? How to treat it? How can homeopathy help you? All of this answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
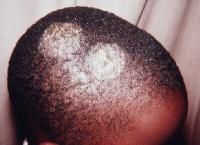
What is Tinea capitis?
Tinea capitis is a fungal infection of the skin on scalp caused by mold-like fungi called dermatophytes. It is also known as ringworm of the scalp, it is mostly seen in persons having minor skin or scalp injury, washing hair less often.
Who are at risk of Tinea Capitis?
It can happen at any age, both male and female are at the same risk. But it is more often in children and it gets better at puberty.
How it is caused by?
It is mostly caused due:
• Minor scalp injury
• Poor hygiene
• Less bathing habits
• Washing hair less often
• Over sweating on the scalp
• Hot weathers
• weak Immune system
• Wet skin for a long time
• Direct contact with infected person.
• infected comb
• Infected cloth
• infected pets.
• Infected brushes or hats
• Diabetes
How to know the presence of disease?
• Redness
• Swelling
• grey Scalp
• dandruff like Dry scaling
• Sores
• Yellow crusts on the scalp
• matted hair
• Low-grade fever.
• Neck lymph nodes Swollen
• Itching
• Brittle or fragile hair
How to confirm Tinea Capitis?
• Physical examination.
• Blood test
• Skin biopsy
• Fungal culture
What others disease are of same symptoms as of Tinea Capitis?
• Alopecia areata.
• Atopic dermatitis.
• Bacterial folliculitis.
• Drug-related rash.
• Impetigo.
• Psoriasis
• Seborrhoeic dermatitis
• Syphilis
How untreated Tinea Capitis get worse?
• Worsened Tinea Capitis may cause:
• Hair loss
• Scarring alopecia
• Permanent scars
• Pus-filled sore
How to manage Tinea Capitis?
• yoga
• balanced diet
• Personal hygiene.
• Cleanliness of scalp
• Usage of personal comb, cloth, and seizure.
• away from pets especially cats.
• Wash towels and cloths in warm soapy water
• Avoid using hats, pillow covers or helmets of infected people.
What are the Homeopathic medicines?
• Agaricus
• Atrium Lappa
• Arsenicum Album
• Baryta Muriatica
• Causticum
• Oleander
• Phytolacca Decandra
For more information, you can visit Wikipedia and eMedicine.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.