
What is Psoriatic Arthritis? What causes this problem? Is it curable? What are the signs and symptoms? How can homeopathy help you? All of this and more answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
Psoriatic arthritis is an autoimmune condition. An autoimmune condition occurs when the body’s immune system mistakenly sends inflammation to normal tissue/structures. In psoriatic arthritis, the inflammation is directed toward the joints causing inflammation swelling, redness, pain and stiffness, and damage.
Psoriatic arthritis can affect any joint of the body but usually affects the large joints, especially those of the lower extremities, distal joints of the fingers and toes, and also can affect the back and sacroiliac joints of the pelvis.
Age/Sex prevalence affected for Psoriatic arthritis
Psoriatic arthritis usually appears in people between the ages of 30 to 50, but can begin as early as childhood. Men and women are equally at risk. Children with psoriatic arthritis are also at risk to develop.
Types of Psoriatic Arthritis
Symmetric psoriatic arthritis: affects several joints in pairs on both sides of your body, like both elbows or both knees
Asymmetric psoriatic arthritis: typically affects only a few joints. They can be large or small and anywhere in your body.
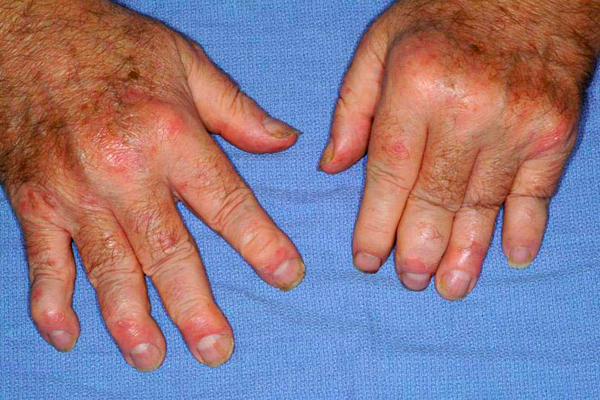
Distal interphalangeal predominant (DIP) psoriatic arthritis: mainly affects small joints at the ends of the fingers and toes, as well as the nails.
Spondylitis affects the backbone. It can cause inflammation and stiffness between your vertebrae
Arthritis mutilans: is the most severe and destructive form of psoriatic arthritis. Fortunately, it’s rare. It damages the small joints in your fingers and toes so badly that they become deformed.
Causes of Psoriatic arthritis
The cause is not exactly known. About 40 percent of patients with psoriatic arthritis have a family history of psoriasis or arthritis. Psoriatic arthritis can also result from an infection that activates the immune system.
Signs and symptoms of Psoriatic arthritis
• Painful, tender, stiff, hot, swollen and red joint.
• Morning stiffness
• Fatigue
• Acne and nail changes (pitting or ridges formation)
Differential Diagnosis of Psoriatic arthritis
• Gout and Pseudogout
• Osteoarthritis
• Reactive Arthritis
• Rheumatoid Arthritis
• Septic Arthritis
Investigation of Psoriatic arthritis
To diagnose psoriatic arthritis, rheumatologists look for swollen and painful joints, certain patterns of arthritis, and skin and nail changes typical of psoriasis.
Laboratory tests
•Elevations of the erythrocyte sedimentation rate (ESR) and C-reactive protein level.
•The Serum immunoglobulin A levels are increased
•Uric acid concentration may be increased.
•Arthrocentesis
Imaging tests
Radiologic features have helped to distinguish psoriatic arthritis from other causes of arthritis.
X-rays.
Magnetic resonance imaging (MRI)
Diet And Management for Psoriatic arthritis
• Physical activity like exercise may help you relax, ease your stress, and sleep better.
Heat and cold therapy
• Hands-on therapies, like massage, acupuncture, and acupressure
• Splints
Treatment of Psoriatic arthritis
– Anti-inflammatory medications (NSAIDs)
– Biologic drug
– Disease-modifying antirheumatic drug
– Immunosuppressant drugs can also reduce psoriasis skin symptoms but can lead to liver and kidney problems and an increased risk of serious infection. The action of these immunosuppressants is to suppress the disease symptoms but their adverse effect on the kidneys and the liver leads to loss of immunity and cause serious skin infections.
Surgical care
Arthroscopic synovectomy
Joint replacement
Arthrodesis and arthroplasty
For more information, you can visit NHS UK and Arthritis Foundation.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.