
What is gangrene? How to manage it? What are the precautions to be taken? What are the signs and symptoms? What is the cause of this disease? How to treat it? How can homeopathy help you? All of this answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
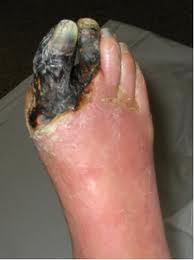
What is Gangrene?
Death of body tissue because of lack of blood supply or bacterial infection is called gangrene. Most commonly it affects the extremities but can also affect muscles and internal organs.
It develops when the death of tissue occurs because of interruption in its blood supply. It may be caused by an infection, injury, or as a complication of a long-term condition that restricts blood flow. Most commonly it occurs in the extremities – the toes, fingers, arms, and legs. The internal organs and muscles also become gangrenous.
What are the types of Gangrene?
• Dry gangrene.
Skin becomes shriveled and dry, color ranges from brown to purplish-blue to black. It occurs slowly and most commonly in people who have any blood vessel disease, such as atherosclerosis.
Wet gangrene.
There is characteristic swelling, blistering and skin appear wet. It can occur after a severe burn, frostbite or injury. Diabetic people are at more risk. The spread of wet gangrene is quick and it can be fatal.
• Gas gangrene.
It affects deep muscle tissues. Skin becomes pale and then changes to gray or purplish-red color. Skin becomes bubbly in appearance and crackling sound is produced when the affected skin is pressed.
• Internal gangrene.
Commonly affected internal organs are intestines, gallbladder or appendix. Blood flow to an internal organ is blocked. It can prove fatal if left untreated.
• Fournier’s gangrene.
The genital organs are affected by this type of gangrene. Fournier’s gangrene occurs as a result of an infection in the genital area or urinary tract and is responsible for genital pain, tenderness, redness, and swelling.
• Progressive bacterial synergistic gangrene.
This develops after an operation. Painful skin lesions develop after one to two weeks of surgery.
What are the risk factors of Gangrene?
Risk factors:
• Age – Old people are at more risk.
• Diabetes – Elevated blood sugar levels damage the nerves, especially in the feet. Elevated blood sugar levels damages blood vessels, resulting in poor blood supply to the lower extremities.
• Vascular diseases – diseases of the blood vessels, such as atherosclerosis and blood clots can result in poor blood flow to various parts of the body.
• Injury or surgery – it will raise the risk of gangrene.
• Weakened immune system – Those with AIDS/HIV, patients receiving chemotherapy or radiotherapy, as well as organ transplant recipients are more susceptible to the complications of infection, which include gangrene.
• Smoking – smoking causes blood vessels to narrow, resulting in less blood flow.
What are the signs and symptoms of Gangrene?
Symptoms of dry gangrene
Dry gangrene develops slowly.
The patients with atherosclerosis and other vascular diseases develop dry gangrene.
• A red line appears on the skin which surrounds the affected tissue.
• When necrosis occurs there may be some pain.
• The area will gradually become numb and cold.
• The area will change from red to brown, to black.
• The tissue shrivels and eventually falls.
Symptoms of wet gangrene
Wet gangrene is more painful as compared to dry gangrene.
• The affected area swells before any tissue dies.
• The skin will change color from red to brown, to black.
• There will be pus and a foul smell.
• Fever
Symptoms of Gas gangrene
Gas gangrene is usually caused by Clostridium perfringens bacteria. The bacterial infection produces the toxin that releases gas. Gas gangrene can become life-threatening.
• The affected area feels heavy and painful.
• The skin may appear to bubble.
• A crackling sound when the area is pressed. This sound is caused by the gas.
• Sometimes there may be a watery discharge which does not usually have a foul smell.
What are the investigations for Gangrene?
• Blood tests to see the number of white blood cells as they are high in gangrene.
• CT scan to examine internal organs.
• Tissue Examination.
• A culture of the tissue or fluid from wounds to identify bacterial infection.
• Arteriogram.
• X-rays.
What is the treatment for Gangrene?
• Antibiotics
• Surgery: Dead tissue is removed surgically; this helps in preventing gangrene from spreading.
• Skin graft: Healthy skin is taken from one part of the patient’s body and spread it over the affected area.
• Amputation: Amputation of the affected body part is done in cases of severe gangrene, for example, a finger, toe, or limb.
• Hyperbaric oxygen therapy
• Maggot therapy
• Blood transfusions: This may help in reducing the infection and speed up the healing process.
What is the prognosis for gangrene?
• Prognosis depends on the type of gangrene, a condition of a patient and how much gangrene is present.
• Death can occur in case of delayed treatment.
What is the complication of Gangrene?
• Disability from the amputation of part or removal of dead tissue.
• Prolonged healing of a wound.
What is the Homeopathic treatment for gangrene?
-Arsenicum
-Crotalus
-Secale
-Carbo vegetabilis
-Lachesis mutus
-Polygonum punctatum
-Sulphuricum acidum
What is the diet and management for gangrene?
• Foot care: if you have diabetes regularly examine your hands and feet for cuts, sores, and signs of infections.
• Avoid Smoking
• Treat cuts promptly: if you cut or graze your skin wash it with warm water and mild soap and keep it clean and dry until it heals.
• Frostbite: if you have been out in the cold for a long time and your skin becomes pale, cold and numb, gets it treated.
For more information, you can visit MedicalNewsToday and Wikipedia.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.