
What is Diabetic Retinopathy? How to manage it? What are the precautions to be taken? What are the signs and symptoms? What is the cause of this disease? How to treat it? How can homeopathy help you? All of this answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
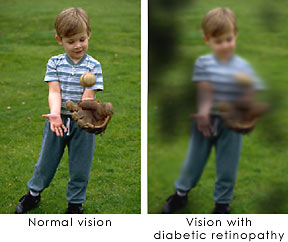
What Diabetic Retinopathy is?
Diabetic retinopathy is defined as the damage to the retina which is caused by the complications of diabetes, which can eventually lead to blindness.
It is a systemic disease which affects up to 80 percent of all patients who have had diabetes for 10 years or more.
This disease results from the microvascular retinal changes.
Which age group are more affected due to diabetic retinopathy?
The diabetic retinopathy develops after 40 years of individuals who suffer from diabetes for long time.
Both sexes are affected due to diabetic retinopathy.
What are the causes of Diabetic Retinopathy?
History of the patient.
Family history of the patient.
Lack of control in levels of sugar.
High blood pressure.
High cholesterol.
Pregnancy.
Tobacco use.
The major cause of diabetic retinopathy is the excess of sugar in the blood.
This excess of sugar in the blood can lead to damage to the tiny vessels.
What is the diabetic retinopathy sign and symptoms?
•Blurred vision.
•Fluctuating vision.
•Dark or empty areas in your vision.
•Vision loss.
•Difficulty with color perception.
•Spots or dark strings floating in your vision.
What are the stages of diabetic retinopathy?
There are 4 stages of diabetic retinopathy. These are:
Mild stage of diabetic retinopathy.
Moderate stage.
Severe stage.
Non proliferative & proliferative stage.
How to Investigate diabetic retinopathy?
Signs to be examined by doctor are as follows
•Presence or absence of a cataract.
•Abnormal blood vessels.
•Growth of new blood vessels and scar tissues.
•Retinal detachment.
•Abnormalities in your optic nerve.
•Swelling, blood or fatty deposits in the retina.
Other investigations to be helpful are as follows
-Fluorescein angiography.
-Optical coherence tomography.
How to Treat diabetic retinopathy?
Treatment steps for diabetic retinopathy are:
•Glucose control.
• Aspirin therapy.
•Ovine hyaluronidase therapy.
•Bevacizumab therapy.
•Laser photo
Medication treatment given is as follows
•Corticosteroids.
•Monoclonal antibodies.
What is the differential diagnosis of diabetic retinopathy?
•Macroaneurysm.
•Diabetic macular edema.
•Ocular ischemic syndrome.
•Retinopathy, diabetic, nonproliferative.
•Retinopathy, hemoglobinopathies.
•Valsalva retinopathy.
•Sickle cell disease.
• Terson syndrome.
•Central retinal vein occlusion.
•Branch retinal vein occlusion.
How to treat diabetic retinopathy homeopathically?
Homeopathy helps symptomatically in this case. Some of the homeopathic medicines which can help in the case. These are:
Phosphorus
Secale cornutum
Syzygium Jambolanum
For more information, you can visit MayoClinic and diabetes.co.uk.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.