
What is Allergic Rhinitis? How to manage it? What are the precautions to be taken? What are the signs and symptoms? What is the cause of this disease? How to treat it? How can homeopathy help you? All of this answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
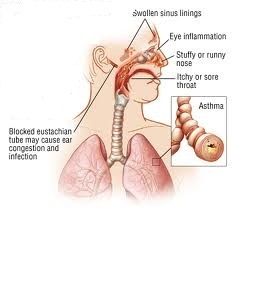
What is allergic rhinitis?
• Allergic rhinitis is an allergic reaction and inflammation of the nose which occurs when the immune system overreacts to inhaled substances, such as pollen.
• It is also known as Hay Fever.
• Allergic rhinitis is a common childhood condition.
• Allergic rhinitis leads to:
-A person having frequent nasal congestion,
-Sneezing,
-itching in the eyes and excessive tear production.
• In some worse cases the allergic rhinitis can lead:
-Asthma
-Sinusitis.
Which age group is more affected due to allergic rhinitis?
• Allergic rhinitis is common in males than females.
• Mainly childhood is affected due to allergic rhinitis.
What causes allergic rhinitis?
• Oversensitive immune symptoms.
• Presence of allergen.
• Tree pollen, in spring.
• Fungus.
• Mold growing on dead leaves.
• Grass pollen, in late spring and summers.
• House mites.
• Animal dander.
• Mold Spores.
Other causes of perennial allergic rhinitis are:
• Cleansers
• Chemicals
• Construction material gases.
• Perfumes
• Cosmetics
• Industrial chemicals
• Cigarette smoke
What are the sign and symptoms of allergic rhinitis?
• Excessive nasal secretion is known as rhinorrhoea.
• A sore throat.
• Nasal congestion.
• Post-nasal drip.
• Swollen nasal turbinates.
• Itchy mouth, throat, ears, and face.
• Fatigue.
• A dry cough.
• Sneezing.
• Red, itchy, and watery eyes.
• Swollen eyelids.
• A headache, facial pain or pressure.
• Partial loss of hearing, smell, and taste.
• Poor concentration.
What is the differential diagnosis of allergic rhinitis?
• Sinusitis (acute and chronic).
Is there any test to b done for allergic rhinitis?
• Diagnosis is based on the history of a patient.
• Skin tests.
• Blood tests for the allergen.
What is the difference between allergic rhinitis and the common cold?
The difference between allergic rhinitis and common cold are:
In case of allergic rhinitis:
• It is caused by allergens.
• In this case generally, do not have a fever or body ache.
• Nasal discharge watery.
• Sneezing.
• Watery eyes.
In case of the common cold:
• It is caused by germs.
• In this case, fever and body aches are present.
• Yellowish greenish thick mucus from the nose.
• Sneezing is infrequent.
• No watery eyes in most of the cases.
How to treat allergic rhinitis?
• Low-dose steroid nasal sprays.
• Decongestant tablets and sprays.
• Antihistamine medications.
• Desensitization immunotherapy.
How to reduce the probability of allergic rhinitis?
• Stay indoors, and close the windows.
• Do not hang laundry outside to dry.
If you have year-round allergies:
• Cover the pillows and mattress with dust mite covers.
• Use blinds instead of curtains.
• Keep pets out of the bedroom.
What are the dietary management for allergic rhinitis?
• Avoid cold food.
• The packed food should be avoided.
• Cooked the food properly because it kills the allergens.
• Intake of Vitamin C it helps to raise immunity.
How allergic rhinitis can be treated with homeopathic medicines?
Homeopathic medicines help symptomatically in this case. Some of the homeopathic medicines which can help in this case. These are:
• Arsenicum album
• Arum triphyllum
• Sanguinaria canadensis
• Allium Cepa
• Gelsemium
• Sabadilla
For more information, you can visit HealthLine and MayoClinic.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.