
What is Dry Eye Syndrome? How to manage it? What are the precautions to be taken? What are the signs and symptoms? What is the cause of this disease? How to treat it? How can homeopathy help you? All of this answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
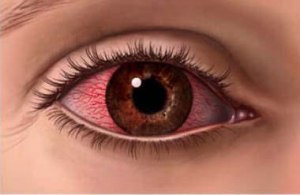
What is dry eye syndrome?
Dry eye syndrome is also known as kerato conjunctivitis sicca (KCS) or keratitis sicca or xeropthalmia is an eye disease caused by dryness of eye which in turn is caused by either decrease in production of tears or due to increased evaporation of tears.
Commonly seen in?
Kerato conjunctivitis sicca is especially seen in older people those aged 40 or older.
People who suffer from autoimmune diseases have a high likelihood of having dry eye syndrome.
Dry eye syndrome is more common in women because of hormonal changes that occur during pregnancy, menstruation, and menopause leading to decreased production of tears.
Causes of Dry eye syndrome?
The two major causes linked to decrease in the adequate tear levels for eyes are as follows:
-Deficient production of tears that is aqueous deficiency state
-An evaporation state leading to evaporation of tears
Aqueous tear deficiency (ATD) is the most common cause of dry eye and due to insufficient tear production. Causes of deficient aqueous production includes:
-Reflex hypo-secretion
-Systemic drugs
-SS (Sjogren disease) dry eye
-Lachrymal gland duct obstruction
Causes behind the evaporative loss of tears are:
-Disorders of the lid aperture
-Low blink rate of eyelids
-MGD (Meibomian Gland Dysfunction)
-Deficiency of vitamin A
Contact lens wearing
-Ocular surface disease
There are different conditions which can lead to less formation of aqueous in the eyes are:
-Non-Sjogren syndrome
There are different types of lachrymal gland deficiencies leading to dry eye syndrome and they are as follows:
-Age-related dry eye
-Congenital alacrima (lachrymal secretory disorders)
-Familial dysautonomia
-Sarcoidosis
-Lymphoma
-AIDS
-Graft vs host diseases
-Lachrymal gland infiltration
-Amyloidosis
-Trachoma
-Lachrymal gland ablation
-Systemic vitamin A deficiency
Medications also hampers aqueous production includes:
-Beta-blockers
-Diuretics
-Anti-cholinergics
-Anti-arrhythmics
-Antihistamines
-Atropine
-Topical Anesthetics
Sign and symptoms of Dry eye syndrome?
Following are the most common symptoms found in patient suffering from dry eye syndrome are:
-Hyperemia
-Mucoid discharge
-Ocular irritation
-Excessive tearing
-Photophobia
-blurry vision
Can dry eyes cause blindness?
No, dry eyes does not cause blindness but can cause blurring of vision, redness, irritation, burning, scratchy feeling in the eyes.
Can dry eyes cause floaters?
Eyes are filled with a gel-like substance known as vitreous humor.Very rarely eye floaters can be seen in case of dry eyes.
Is it dangerous to have dry eyes?
When left untreated, dry eye syndrome can permanently harm your vision. It can cause sensitivity to light as well as blurred vision.
How to investigate Dry eye syndrome?
Tests to be done are as follows
-Tear break up time
-Epithelial staining
-Schirmer test
-Test to quantify tear components
How to treat Dry eye syndrome?
Pharmacologic therapies given to the patients with dry eye syndrome are as follows
-Artificial tear substitutes
-Gels and ointments
-Systemic immuno-suppressants
Along with all these eye protections is very important in dry eye syndrome and can be done by the use of following
-Use silicone rubber lenses
-Highly oxygen-permeable lenses
Complications of Dry eye syndrome?
Complications of dry eye syndrome are as follows:
-Sterile or infectious corneal ulceration
-Occasionally corneal perforation may occur
-Vision loss may occur
How to manage Dry eye syndrome with homoeopathic medications?
-Veratrum album
-belladonna
-asarum europium
-causticum
-chamomilla vulgaris
For more information, you can visit WebMD and eMedicine.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.