
What is Crohn Disease? How to manage it? What are the precautions to be taken? What are the signs and symptoms? What is the cause of this disease? How to treat it? How can homeopathy help you? All of this answered, in this post and of course our doctors always there to help you. Just fill in your details in the form down below and we will answer all your questions for FREE!
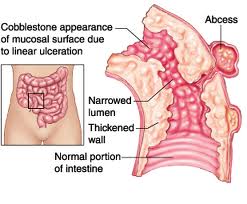
What is Crohn’s disease?
Crohn disease is also known as Ileitis or Enteritis. In Crohn’s disease inflammation of digestive tract occurs that results in ulceration of small and large intestine.
Crohn disease is closely related to ulcerative colitis.
But the two are different in the following ways:
• In Crohn’s disease inflammation occurs in colon, rectum, small intestine and occasionally stomach, mouth, and esophagus.
But in Ulcerative colitis inflammation occurs only in the colon.
• In Crohn disease, deeper layers of bowel are involved.
In Ulcerative colitis superficial layer of bowel is involved.
Crohn’s disease and Ulcerative colitis together are known as Inflammatory bowel disease.
Basics:
Small erosions occur on the surface of bowel that results in deep ulcers which causes scarring and stiffness of bowel. As the disease progresses narrowing and obstruction of bowel occurs. Due to obstruction the food and fluid from the stomach cannot pass into colon resulting in severe abdominal cramps, nausea, vomiting and abdominal distention.
Deep ulcers can perforate the walls of small intestine and colon as a result of bacteria from bowel spread to adjacent organs and cause infection.
What are the causes of Crohn’s disease?
The exact cause of the disease is unknown. Studies have suggested that heredity and malfunctioning immune system may be responsible for Crohn’s disease.
Risk factors include:
• Family history.
• Age below 30 years.
• Smoking.
• Appendectomy.
What are the symptoms of Crohn’s disease?
Sometimes the patient may remain asymptomatic. The symptoms during the active stage of disease are:
• Severe abdominal pain.
• Loss of appetite.
• Pain while passing stool.
• Diarrhea or constipation.
• Weight loss.
• Fever.
• Fatigue.
• Rectal fistula.
• Sore mouth because of ulcers.
How to investigate Crohn’s disease?
Blood test
• Liver function test
• Fecal occult blood test
• Colonoscopy
• Flexible sigmoidoscopy
• CT scan
• MRI
• Barium enema
• Capsule Endoscopy.
• Double balloon endoscopy.
What are the risk factors involved in Crohn’s disease?
• Intestinal bleeding
• obstruction of the small intestine
• liver diseases: hepatitis, jaundice, cirrhosis
• fistulae
• abscess formation
• rupture of the intestine
• painful eye conditions
• pain and stiffness in the joints
What treatment is advised for Crohn Disease?
Medicines that may be prescribed include:
• antibiotics
• corticosteroids
• aminosalicylates.
Surgery: It is needed if symptoms do not respond well to medicines. In some cases surgical removal of the entire intestine is necessary.
How to manage Crohn’s disease?
• Frequent small meals at short intervals.
• Drink plenty of water.
• Avoid foods high in fiber content.
• Avoid fried foods and sauces.
• Limit your consumption of dairy products.
What is the prognosis of Crohn Disease?
The patient sometimes remains asymptomatic with episodes of flare-ups. The disease is incurable, only symptomatic relief is given by medicines.
Medicines should be continued for a long time to stop symptoms from returning.
For more information, you can visit MayoClinic and MedicalNewsToday.
We have a strong web presence all across the globe with patients in major countries like United States, Australia, United Arab Emirates, Canada, United Kingdom, most European countries, & even smaller counties like Uganda, Nepal, Bangladesh and many more.
We have a very efficient team of doctors which includes the right combination of highly experienced doctors and the doctors of the new age.
Our main aim is to make the patient comfortable so that the case can be taken with ease and the patient be treated properly.
** The text on this website is sourced from websites like emedicine and/or other verified material by government agencies around the globe along with valuable inputs and additions by our team. The content of this page is proofread and updated by the team of doctors, every once in a while, to provide the most accurate information.